Within the Medi-Cal managed care program, California currently uses a variety of different models to deliver care. In this post, we will review the Six (6) Medi-Cal Managed Care Models in California, how each is organized, and the list of states participating in each model.
Additionally, we will walk you through Medi-Cal Eligibility and Enrollment and what services are covered by Manage care plans.

Medi-Cal in California
California’s Medicaid program, Medi-Cal, is the largest state Medicaid program in the nation.
The Medi-Cal program provides health coverage for almost one-third of California’s more than 39 million residents.
Additionally, Medi-Cal is a key source of health coverage in the state and the main source of coverage for low-income children, adults, and people with disabilities.
Also, Medi-Cal provides wrap-around insurance coverage for many elderly Medicare beneficiaries in the state.
The transition from Fee for Service Model
Over the last several decades, California Medi-Cal has been transitioning away from a fee-for-service (FFS) payment and delivery system to one that relies on managed care plans.
Under the FFS system, beneficiaries could see any provider who accepted Medi-Cal, and providers were reimbursed for each individual service or visit.
However, under managed care, the state contracts with health plans to deliver Medi-Cal benefits to enrollees in exchange for a monthly premium, or “capitation” payment for each enrollee.
The plans are accountable for and at financial risk for providing the services in the contract.
California was the first state to pilot managed care in Medicaid, beginning in the early 1970s.
The Growth of Medi-Cal Managed Care Models
Over the last few decades, several models of managed care delivery and financing systems have been developed in different counties of the state.
Currently, in most counties in California, the Department of Health Care Services (DHCS) contracts with one or two managed care plans (MCPs) to deliver services to Medi-Cal enrollees.
In November 2010, the Department of Health Care Services (DHCS), California’s Medicaid agency, expanded the state’s managed care to seniors and people with disabilities enrolled in Medi-Cal.
As of 2022, approximately 10.8 million Medi-Cal beneficiaries in all 58 California counties receive their health care through six main models of managed care.
This accounts for 84% of Medi-Cal enrollees.
Types of Medi-Cal Managed Care Models in California
Within the Medi-Cal managed care program, California currently uses six different models to deliver care.
The six Medi-Cal managed care models are:
- Two-Plan
- County Organized Health Systems (COHS)
- Geographic Managed Care (GMC)
- Regional Model (RM)
- Imperial
- San Benito
Currently, a total of 24 plans contract with the Department of Health Care Services (DHCS) to provide Medi-Cal managed care services to beneficiaries.
Of these, 16 are local health plans (also known as LHPC).
The 16 LHPC member health plans participate in the Two-Plan, COHS, and GMC models, covering over 70% (7.5 million) of all Medi-Cal beneficiaries in California.
Below is a distribution of Medi-Cal enrollment by managed care model as of 2019:
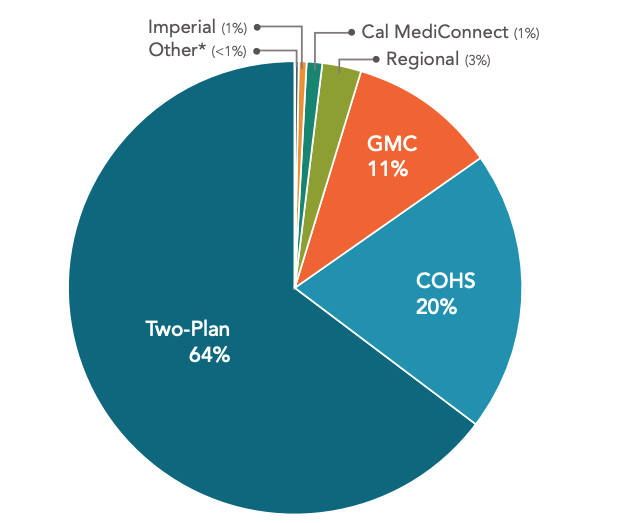
We have provided below details on how each of the six managed care models works and participating counties:
Two-Plan Managed Care Model
Under the Managed Care Two-Plan Model, the Department of Health Care Services (DHCS) contracts with two managed care plans to provide medical services to most Medi-Cal recipients in each of the participating counties.
The Two-Plan Model offers enrollees a choice between one commercial plan and one “Local Initiative” public plan.
Local initiative plans, which are initiated by a county board of supervisors, are operated by a locally developed comprehensive managed care organization.
Commercial plans are operated by non-governmental managed health care organizations. Medi-Cal recipients may enroll in either plan.
There are 14 counties participating in the Two Plan Managed Care Model:
- Alameda
- Contra Costa
- Fresno
- Kern
- Kings
- Los Angeles
- Madera
- Riverside
- San Bernardino
- San Francisco
- San Joaquin
- Santa Clara
- Tulare
County Organized Health System (COHS) Model
First established 30 years ago, the County Organized Health System (COHS) plans were pioneers in managed care that specialize in serving Medicaid (Medi-Cal) populations.
COHS allows for enrollment in a single, local public health plan. The plan is created and administered by a County Board of Supervisors.
There are 22 counties participating in the COHS Managed Care Model:
- Del Norte
- Humboldt
- Lake
- Lassen
- Marin
- Mendocino
- Merced
- Modoc
- Monterey
- Napa
- Orange
- San Luis Obispo
- San Mateo
- Santa Barbara
- Santa Cruz
- Shasta
- Siskiyou
- Solano
- Sonoma
- Trinity
- Ventura
- Yolo
Geographic Managed Care (GMC) Model
The Geographic Managed Care (GMC) model was established to provide medical care for Medi-Cal recipients in specified aid code categories for a capitated fee.
This model is available in Sacramento and San Diego counties. The San Diego plan operates as “Healthy San Diego.”
Regional Model (RM)
The Regional Model was developed for the rural expansion of Medi-Cal managed care plans.
The Department of Health Care Services (DHCS) contracts with two Commercial plans to provide services in each county.
San Benito is the only exception where beneficiaries can choose either the managed care plan or (fee-for-service) Medi-Cal.
The Regional Model serves beneficiaries in 28 rural counties:
- Alpine
- Amador
- Butte
- Calaveras
- Colusa
- Del Norte
- El Dorado
- Glenn
- Humboldt
- Inyo
- Imperial
- Lake
- Lassen
- Mariposa
- Mendocino
- Modoc
- Mono
- Nevada
- Placer
- Plumas
- San Benito
- Sierra
- Siskiyou
- Sutter
- Tehama
- Trinity
- Tuolumne
- Yuba
Imperial Model
This model only operates in Imperial County where DHCS contracts with two commercial plans.
San Benito (Voluntary) Model
This model only operates in San Benito County where DHCS contracts with one commercial plan.
Below is a map from the Kaiser Foundation showing the six models by county.
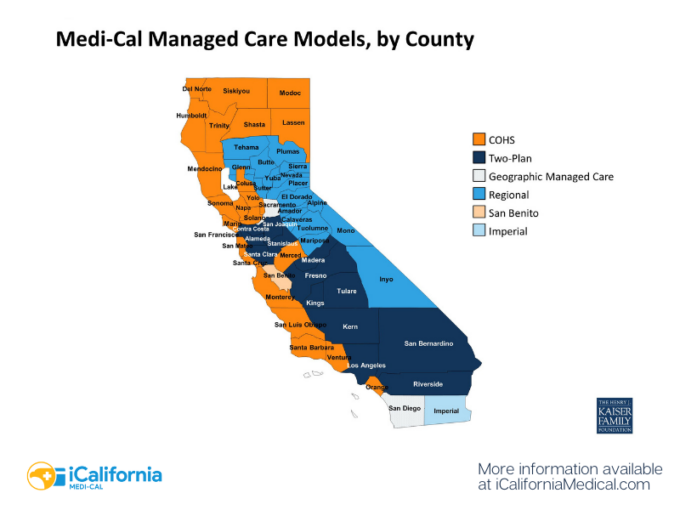
Medi-Cal Eligibility and Enrollment
In California, there are two primary ways of determining Medi-Cal eligibility – either through County Social Services Agencies (SSAs) or through the California Healthcare Eligibility, Enrollment, and Retention System (CalHEERS).
The CalHEERS is the single point of entry for health coverage required under the federal Affordable Care Act (ACA).
Applications can be completed online, in person, or by mail.
In addition, numerous community-based organizations and healthcare providers around the state provide assistance in applying for Medi-Cal.
Application Processing
Once an application has been submitted, eligibility and processing are done by county SSA staff.
If the county SSA staff determines that an applicant is eligible, the beneficiary is enrolled in Medi-Cal and is issued a Benefits Identification Card (BIC).
In counties where the County Organized Health Systems (COHS) care model is used, all beneficiaries are mandatorily enrolled in the single COHS plan.
However, in San Benito County where there is only one health plan available, beneficiaries may enroll in that plan or choose to receive Medi-Cal fee-for-service.
In all other counties where there are at least two health plans, beneficiaries receive a choice packet from the Department of Health Care Services (DHCS) to use to select a plan.
Any beneficiaries who do not select a plan are automatically assigned to one.
Beneficiaries may change plans for any reason or if they move to another county by contacting DHCS’s Health Care Options (HCO) program by phone or by mail using an Enrollment Choice Form.
Choosing a Primary Care Provider
Once a beneficiary enrolls in a plan, the beneficiary chooses a primary care provider (PCP) who is either a doctor or clinic that is part of the health plan’s network.
If no PCP is selected, one will be assigned.
However, beneficiaries may change PCPs at any time by calling the health plan’s member services department.
Additionally, beneficiaries receive a provider directory or can access the provider directory online, to see complete information about the providers who are contracted with the health plan.
This information includes address and telephone number, hours, available services and benefits, languages spoken, and after-hours phone number.
What is Covered by Medi-Cal Care Plans
The Medi-Cal program offers a comprehensive set of health benefits at no cost to the beneficiary.
There are no premiums or co-payments.
However, some Medi-Cal benefits are not included in the health plans’ contracts and are “carved out” of managed care.
This means that they are administered by another entity other than the health plan.
In general, these carve-out benefits include:
- Dental benefits
- California Children’s Services
- AIDS Drug Assistance Program
- Specialty mental health
- Drug Medi-Cal
- In-Home Supportive Services (IHSS)
In many instances, the carved-out benefits are administered by the State or county agencies.
Medi-Cal Managed Care Models Summary
We hope this post on the six Medi-Cal Managed Care Models was helpful.
Questions?
If you have further questions about Medi-Cal, please let us know in the comments section below.
Be sure to check out our other articles about Medicaid, including:


